Patient Testimonials
Bridget’s Story
Patient Information
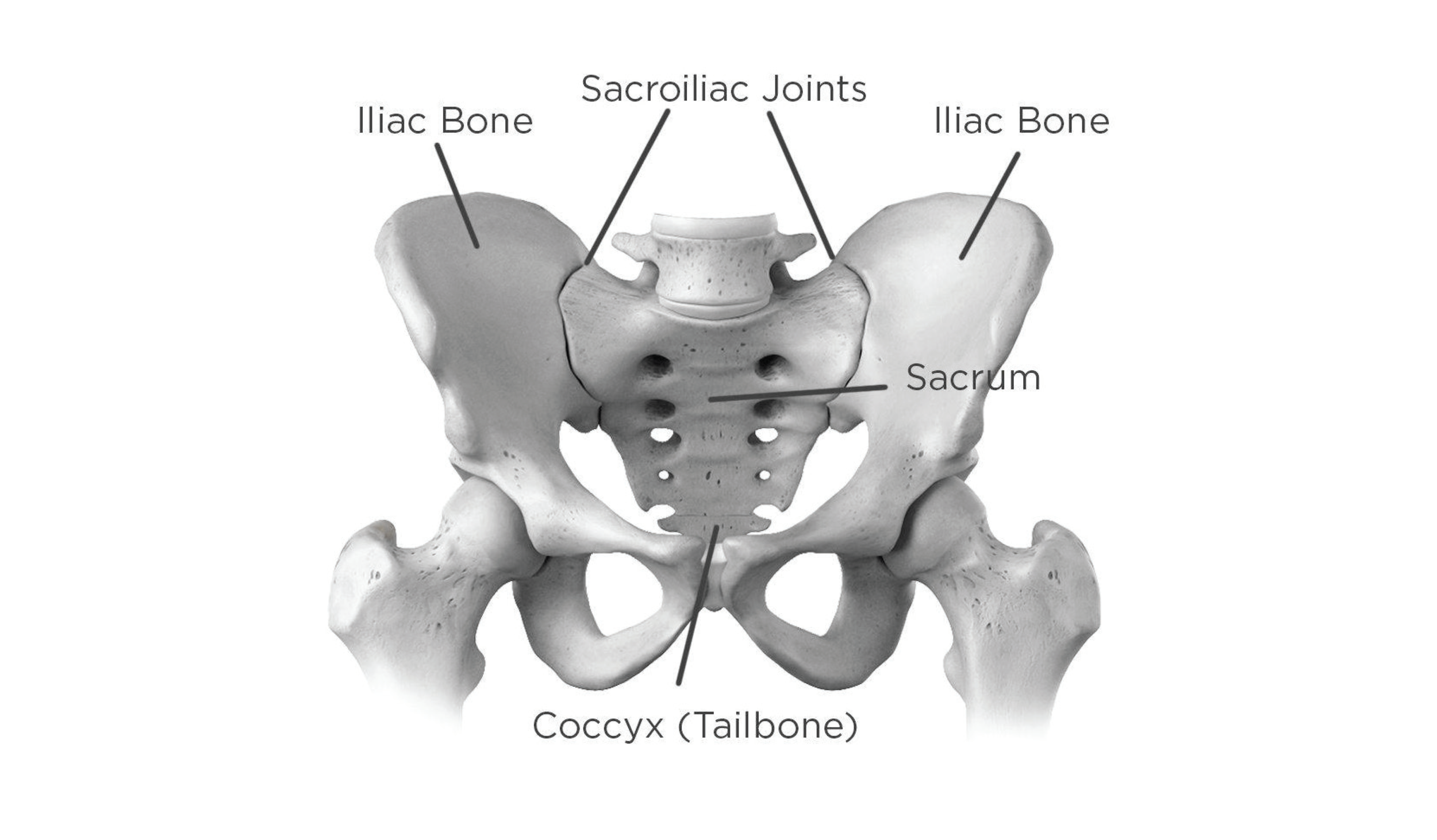
SPINE & PELVIC ANATOMY
The sacroiliac joint (SI joint) connects the sacrum (triangular bone at the bottom of the spine) with the pelvis (iliac bone that is part of the hip joint) on each side of the lower spine. The SI joint provides stability and bears the load of the upper body by transferring its weight and forces through the pelvis to the legs. This joint is essentially the shock absorber of the body when activities are being performed. Typically this joint does not have much movement.
Your SI Joints
The SI Joints have numerous nerve endings and when degneration or inflammation affect their ability to move properly it can be very painful.
DIAGNOSING
There are several primary causes of spine problems. The majority of the symptoms are caused by disc, bone, or ligaments pressing onto the nerve roots or cord.
Why is the si joint causing pain?
There are several reasons why the SI joint can start causing pain. Injuries are the most common cause, while degenerative changes can lead to pain as well. Other causes that contribure to SI joint pain include but are not limited to: Rheumatoid Arthritis (RA), deformity such as pelvic tilt and obliquity, limb length inequality, or instability with motion of the pelvis.
DIAGnOSIS: IS THE SI JOINT CAUSING YOUR LOW BACK PAIN?
Do you have trouble sitting for long periods of time with pain?
Do you have to shift from side to side while sitting?
Do you have trouble sleeping comfortably at night?
Do you have pain in your buttocks while climbing stairs?
Does your pain get worse when getting in and out of a car?
Does driving over a bump in the road increase back and/or buttocks pain?
Do you have trouble and is it painful standing on one leg for a prolonged period of time?
Does your leg feel like it wants to give out when stepping?
SI Joint Exam
Physical Examination
Diagnosis to rule out other sources of pain
Diagnostic imaging (X-ray, CT, MRI)
Provocative Tests
Fortin Finger Tests
Diagnostic injections of the SI joint
Diagnostic Tests & Imaging
Effective training methods and ways of diagnosis are not commonly practiced by many doctors. Provocative tests as well as diagnostic injections can be conducted to better pinpoint the source of the pain. These provocative tests involve manipulating the body in a way to replicate the specific pain that you are experiencing. Because the SI joint is not as mobile as your shoulder or hip, your doctor will need to manipulate the joint in a way that will induce your pain symptoms. In order for the test to be conclusive several of the manipulations will have to replicate your pain. CT-Scans and MRI’s are other tools that can be used to better diagnose SI joint related problems.
In addition, X-rays, a CT scan, or MRI may be helpful in diagnosis. It is also important to remember that more than one condition (like a disc or hip problem) can co-exist with SI joint problems and your doctor will need to check for other factors that may be causing your symptoms.
CONSERVATIVE TREATMENT OPTIONS
Try the following conservative care options before considering surgery.
Non Steroid Anti-Inflamatory (NSAIDS)
Physical Therapy (6 - 8 weeks IJ stabilization program)
Family Assisted Correction
Self-Mobilization Techniques
External Fixation (belt/tape)
Steroid Injections (up to 3 a year)
If these conservative options do not help with pain, your doctor may recommend SI joint fixation surgery as the next step
MIS Joint Fusion
with SImpact

WHAT TO EXPECT AT YOUR Physician visit
Doctors are trained on effective ways to test for SI joint pain. Provocative tests as well as diagnostic injections can be conducted to better pinpoint the source of your pain. One of the most conclusive tests for SI joint pain are diagnostic injections.
What to expect after sI Surgery
Your physician may recommend you to use a brace for a short period of time. Under supervision of trained medical professionals, your physician may ask you to sit, stand or walk within 24 hours of the surgery. After discharge from the hospital, you can expect to have limitations on your activities as determined by your health care provider. Your physician will prescribe any necessary pain medication and will provide instructions regarding exercise, wound care and appropriate activity.
FREQUENTLY ASKED QUESTIONS
CAN I SHOWER AFTER SURGERY?
Ask your physician as to any showering restrictions that may apply to your particular situation.
WILL I HAVE A SCAR?
Ask your physician to discuss the incisions made during your procedure. Small scars at the surgical site are common.
WHEN CAN I DRIVE?
You may be asked to not drive for a period of time after the surgery. Your physician will instruct you as to when you can drive again.
WHEN WILL I BE ABLE TO RETURN TO WORK?
Individual recovery time will vary. Other factors such as individual job duties and physical requirements will apply. Consult your physician for specific recommendations.
HOW LONG WILL I HAVE RESTRICTED ACTIVITIES?
You can expect to have activities limited in a period usually reaching 6 months post operation. Your physician will give you specific instructions related to restricted activity.
Find a Doctor Near You!
Fill out the below information and we will send you local doctors in your area!
*Disclaimers:
1) The Life Spine “Find a Doctor” site is for informational purposes only. Physicians who are listed in this finder have demonstrated a minimum level of proficiency using Life Spine’s technology. No physician has paid a fee or received a fee to be listed.
2) Life Spine does not recommend or endorse any particular physician or course of treatment for your condition.